Our vision is to provide comprehensive care. We also benefit from our collaboration with doctors, says Mgr. Kateřina Jinochová, head physiotherapist at the Orthotes Clinic
 The Orthotes Clinic is a facility that offers services in a combination of fields, from orthopaedics, traumatology and rehabilitation, to physiotherapy. And the clinic’s head physiotherapist is Mgr. Kateřina Jinochová, who combines her sessions with patients with teaching students, organising courses and working with top athletes. She recommends Alignment Socks for both prevention and treatment, and even wears them herself. So what can you expect if you visit the clinic as a patient?
The Orthotes Clinic is a facility that offers services in a combination of fields, from orthopaedics, traumatology and rehabilitation, to physiotherapy. And the clinic’s head physiotherapist is Mgr. Kateřina Jinochová, who combines her sessions with patients with teaching students, organising courses and working with top athletes. She recommends Alignment Socks for both prevention and treatment, and even wears them herself. So what can you expect if you visit the clinic as a patient?
About physiotherapy at the Orthotes Clinic
The Orthotes Clinic was established in 2009 and is situated at Budějovická in Prague 4. In our facility we provide orthopaedic and trauma care, rehabilitation and physiotherapy.
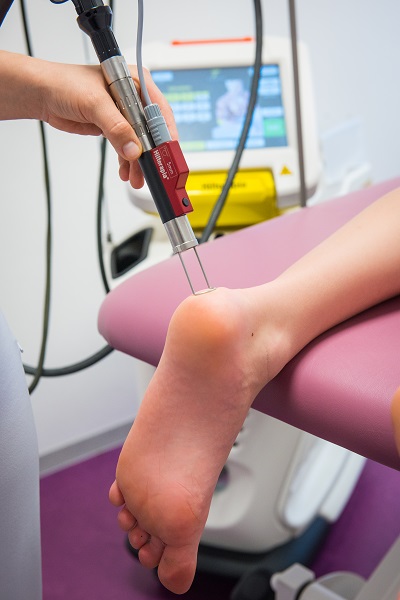
The physiotherapy department provides care across the entire field of physiotherapy, focusing primarily on orthopaedic diagnostics (the back, hips, knees, flat feet, hallux valgus, and so on). Since 2014 we have also been using HILT® – HILTherapy, or high-intensity laser therapy, which is very effective at treating problems such as inflammation of the Achilles tendon, heel spurs and plantar fasciitis.
What aspect of physiotherapy do you specialise in?
At our clinic I personally specialise primarily in patients with back, leg and foot pain, as well as orthopaedics for people following an accident or an operation. I most frequently use Fascial Manipulation (the Stecco Method), neurophysiology-based methods, kinesio taping, Blackroll and podoscopy.
The majority of my patients are professional athletes (ice hockey, MMA, triathlon, athletics, runners, etc.). Outside the clinic, I’m also an external lecturer in physiotherapy at the Faculty of Biomedical Engineering of the Czech Technical University. I find my work with students very satisfying, as it’s highly rewarding to pass on experience and inspire promising young future physiotherapists. I’m also a Blackroll trainer for the Czech Republic. In my spare time, I’m the administrator of the Physiotherapists in Practice group on Facebook, where there are now over 4300 physiotherapists and where we strive to share practical experience and help one another. Or I promote the motto “sharing = caring”.

Do you often find yourselves “passing on” patients within the clinic?
Yes, we do. That’s the basis of our vision – comprehensive care. We examine a patient at the orthopaedics department and, if they’re indicated, we send them on to physiotherapy. We can discuss patients with doctors, and doctors can also receive information about the results of physiotherapy treatment and how well the patient cooperates during autotherapy, and then decide on the next course of treatment, follow-up imaging examinations, and so on.
What deformities of the foot do you most commonly encounter?
Generally, patients come to us with various types of foot pain. Most of them claim that they have very flat feet, because they’ve been told that by someone at some point. However, the cause of their pain generally lies elsewhere. By means of podoscopic, aspect and palpation examinations we find, for instance, that the patient does not have flat feet at all, and also that the pain may originate from higher up (the knee, hip, or perhaps the spine).
So, patients most often come to us with flat feet, hallux valgus or hallux rigidus, pains in the Achilles tendon, a heel spur, plantar fasciitis, hammertoe, Morton's neuroma or leg pain caused by a root irritation (such as discomfort resulting from a certain projection of pain from a spinal disc herniation).
Is it true that these days people are more concerned about the health of their feet than they used to be? If so, why?
I guess it is true. It’s important to realise that humans were predestined (generally speaking) to walk through a forest-steppe landscape, gathering fruit from trees and hunting animals. Human development probably did not take account of us spending 8 hours a day sitting in an office chair and then rushing off to exhaust ourselves in the gym or go for a long run. Our natural movement has become much less frequent (long walks), as nowadays people tend to travel even just a few hundred metres by car or public transport. Overall, we move very little compared to the hours we spend sitting down. And all this is not good for our entire musculoskeletal system, let alone our feet.
Also, there didn’t use to be such a wide range of quality footwear available. People wore what they could get. There’s now a wide choice of footwear, from high-heeled court shoes, through cushioned or soft and hard shoes, as well as sports footwear designed for a specific sport, to things such as barefoot shoes. Greater awareness about quality footwear or shoe size also helps (people often wear shoes that are too small or too narrow).
Nowadays it’s more common for people to go for regular pedicures or use special foot creams and sprays. In our clinic I’ve also seen a patient come in with heel pain. An examination showed that the pain was caused merely by excess strain on the back part of the sole, as it couldn't deflect off the big toe when the patient was walking. He had an overgrown toenail, so he wasn't even able to stand and put weight on his feet evenly without straining the heel. So, a pedicure is also an important part of foot care and can cure certain problems.
Patients being well informed by their doctor or physiotherapist, and a general effort to improve foot care and prevention in particular also play an important role. Special attention to the feet should be given to patients with diabetes mellitus, who suffer from diabetic foot syndrome.
What does a person need to do for you to examine them? Especially if they are unsure which department of the Orthotes Clinic to contact?
Patients should first contact the clinic reception and describe their problem, after which the receptionist will make an appointment for them at the relevant department. We are then happy to examine the patient and propose a course of treatment to cure the problem.
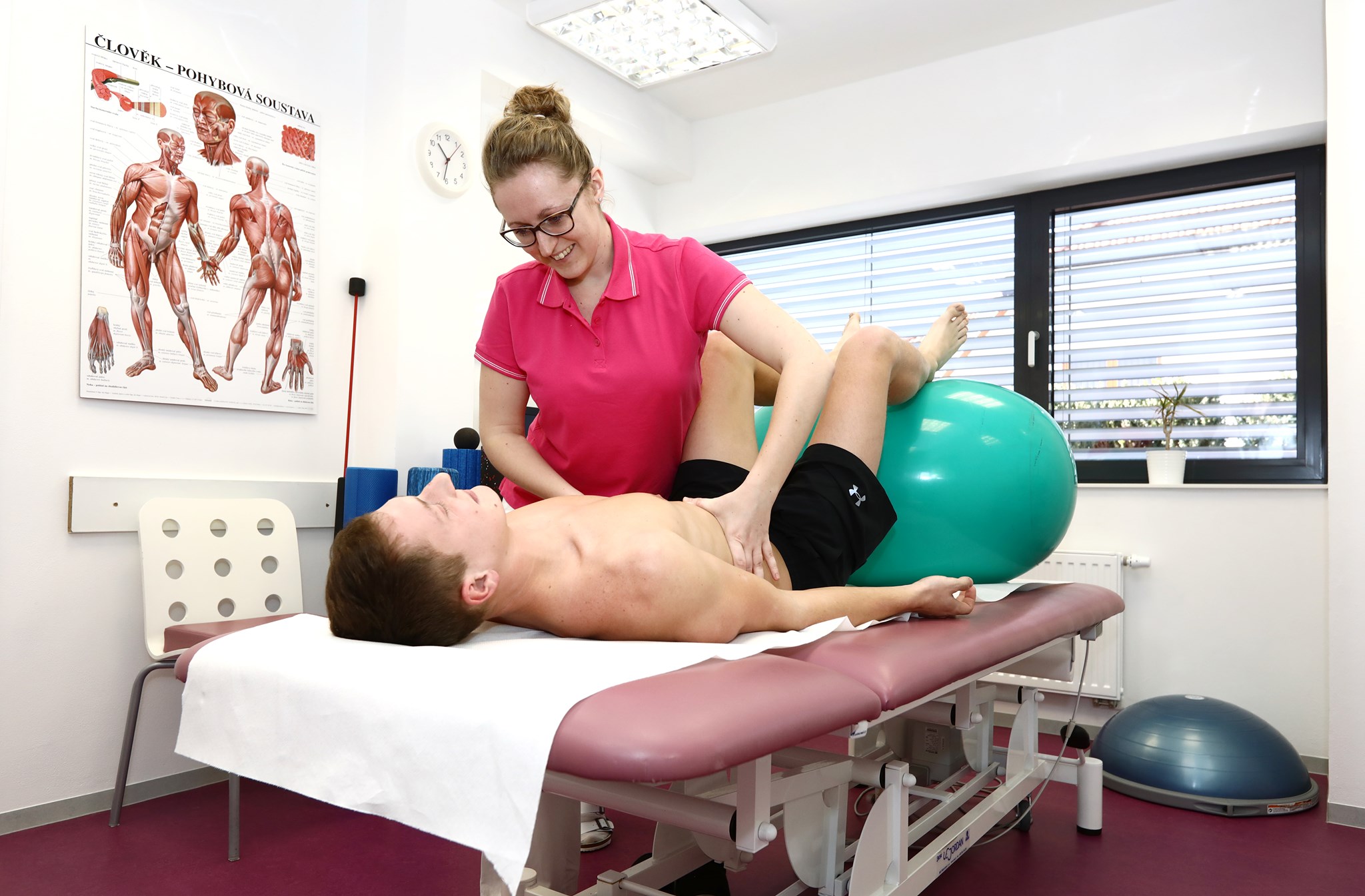
What happens during your first meeting with the patient?
The patient comes for an examination, where they first describe their problem, after which we go over their medical history; this is followed by an aspect (visual) and palpation (touch) examination. We can also carry out a podoscopic examination, which is a great help in diagnosing the problem. We perform special tests, too, depending on what the patient’s complaint is. After that, we determine the cause of the problem and propose a course of treatment.
If necessary, we consult the matter with doctors from the Orthopaedics Department, and look at the results of examinations using imaging methods (such as an X-ray or ultrasound). Finally, we start actual physiotherapy with the patient, as well as autotherapy and changes to their movement and exercise habits or footwear/insoles.
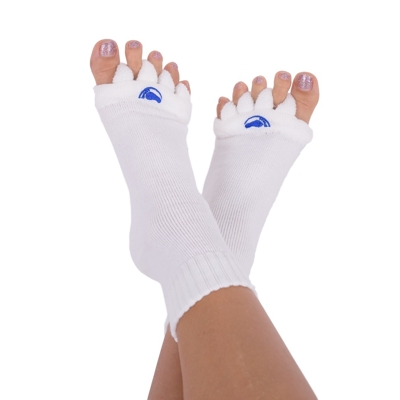
Do you recommend Alignment Socks to your patients? Do you have personal experience with them?
I think Alignment Socks are an excellent aid, both in preventing and treating various diagnoses. From tired, swollen feet, as Alignment Socks work very well to reduce swelling and improve circulation, through to disorders such as halluxes, hammertoes, pain in the metatarsal bones, plantar fascia inflammations, heel spurs, inflammation of the Achilles tendon and other diagnoses that Alignment Socks are excellent at helping to treat. Here, I like to combine them with elements of physiotherapy (active exercises, Blackroll, kinesio taping, and others). Nevertheless, I’d like to stress that wearing Alignment Socks alone will not cure the patient’s problem. They’re just one piece in the overall jigsaw, which needs to be put together in order to alleviate or cure the patient’s ailment.
I myself like to wear Alignment Socks, partly because I’m on my feet all day and I exercise a lot with patients. My feet used to feel really heavy and tired after a long day; wearing Alignment Socks combined with active physiotherapy elements gave me some relief.
What do you think is their greatest benefit?
I personally think that their greatest benefit is that they are “non-invasive” and can be taken off if you feel any discomfort. However, I recommend starting to wear them gradually, not inserting toe separators too deep right at the beginning, and really just relax in them to enjoy the satisfaction they give. Wearing them generally reduces tension in the foot, relieves pain, makes the foot feel rested and relaxed, and eases any imaginary tension and the sensation of a burden on the feet.

What do you enjoy most about your work?
The diversity. No patient is the same; each case is individual, and I try to find the cause of the problem. My aim is to solve the puzzle, as it were, i.e., not just to deal with the consequence of the problem, but to find its true root and completely eliminate it. By combining this with teaching students at the faculty, working with patients in the surgery, including outings with sportspeople and passing on my experience to other physiotherapists on Blackroll courses, my work is constantly rewarding, diverse and out of the ordinary. And I sincerely believe that it will continue to be for a long time yet.