Be alert for diabetic foot syndrome (DFS)

It starts inconspicuously. Cracks or abrasions on the feet start taking longer to heal, accompanied by tingling in the foot and occasional pain. These may well be the symptoms of a condition called diabetic foot. How is DFS recognized and treated and can it be prevented? We look at this in the following sections.
What is DFS and what are the symptoms?
Diabetic foot syndrome is a disease that affects the lower limbs, especially the soles of the feet, heels, big toes and around the toes. Its symptoms include reddened skin, visible foot ulcers, cracks, or abrasions and blisters that do not heal. Because of disruption to blood vessels and nerves in the lower limbs, this dysfunction prevents enough blood getting to the lower limbs and leads to the first symptoms described above. If left untreated, other complications can arise that are far worse.
If DFS is not treated in time, extreme cases carry the risk that the toes or entire limb may have to be amputated. In more than half of these cases, simple steps taken in time can prevent amputation. In the advanced stage of DFS, diabetic ulcers appear on the foot, which take a long time to heal. Patients are also at risk of infectious diseases and tissue necrosis setting in. DFS also increases the mortality of people suffering from diabetes.
The main risks leading to the onset of DFS
The main causes of DFS are a combination of several factors, the main ones being cigarette smoking, high blood pressure, genetics, age and diabetes. Lifestyle is also related to this.
How to treat DFS
Treating DFS depends on the stage the disease has progressed to. The most important matter is stopping the disease from developing, i.e. slowing down the spread of symptoms. In the case of ulcers, it is necessary to relieve the feet and reduce their load, and especially limit long periods of standing or walking. In some cases, wearing diabetic footwear may be required. In extreme cases, your doctor may prescribe crutches, a wheelchair or even bed rest.
It is important that the patient eliminates the risk of injury, abrasions and other damage to the feet as much as possible. Injury can lead to the damage or infection spreading. Treatment is always administered by a doctor, who may also recommend a change in lifestyle. Each change should be closely monitored during treatment. You should therefore check your feet regularly and immediately report any changes to your doctor, who will adapt the treatment to the course of the disease.
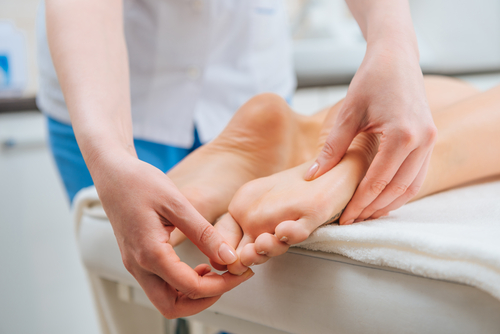
Tools for healing wounds may also be used, depending on the extent of the disease. These range from wound dressings to, for example, laser or ultrasound therapy. If an infection develops, doctors usually prescribe antibiotics. In the case of necrotic wounds, the necrotic part must be surgically removed. Finally, the advanced stage of the disease carries the previously mentioned risk of leg amputation.
Proper foot care is also important during treatment. You should not expose your feet to excessive heat or cold, soak them in water for a long time or walk barefoot. Hygiene and preventing fungal diseases are also very important. After proper washing, dry your feet thoroughly, including the interdigital spaces.
Preventing DFS
The basis of prevention is eliminating the factors that contribute to the onset or spread of the disease. You should therefore not smoke cigarettes, overload your legs or keep them in a damp environment. By contrast, you should maintain sufficient blood circulation, which can also be helped by regularly wearing The Original Foot Alignment Socks.

In addition, keep your feet dry, wear spacious and comfortable shoes that don’t cramp your feet, and don’t forget to let them regenerate as much as possible. You only have one pair of feet, and if you want them to accompany you reliably for as long as possible, you need to take proper care of them. Of course, you cannot influence factors such as age or genetics, but every means of prevention makes sense.